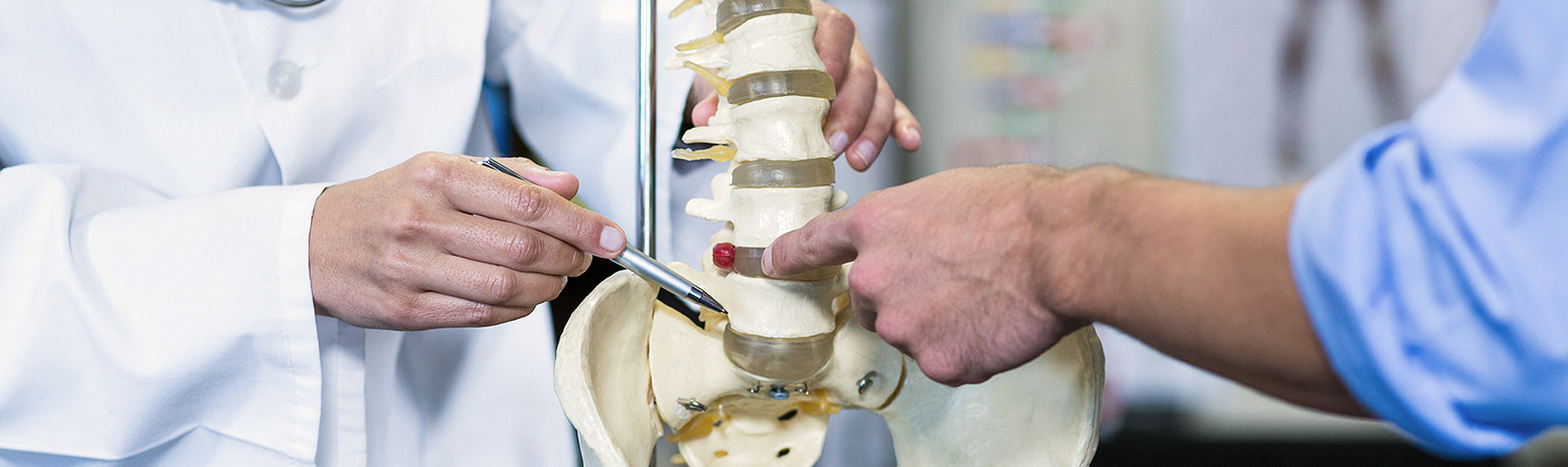
Overview
The term herniated disc describes the condition when the intervertebral disc is injured, and its contents are bulging or protruding into the spinal canal. The terms slipped disc, ruptured disc, bulging disc, disc protrusion, and extruded disc, among others, all mean herniated nucleus pulposus (herniated disc), which is the proper medical term. The first scientific description of a herniated disc first appeared in 1934 in the New England Journal of Medicine. The article described the phenomenon of back pain (lumbago) and radiating leg pain (sciatica) occurring because a spinal nerve in the back was compressed by a herniated disc. Epidemiologic studies have shown that a large percentage of patients with back pain have sustained a disc injury, especially if the patient has accompanying radiating leg pain (sciatica).
|
|
Causes
Although there is an extensive of list of risk factors for the development of back pain (and disc problems), a disc injury can occur in almost any person. It occurs most frequently in people age 20-50 years old, and affects men and women equally. The cause of a herniated disc injury can often be identified if someone develops severe back pain and sciatica immediately after an accident or lifting a heavy object. However, most people presenting with a disc injury do not recall a specific event that provoked their pain, and the actual cause is indeterminate. People who perform heavy labor (and utilize proper lifting techniques) or participate in sports have nearly the same rate of injury as people who do not.
Symptoms
Patients may present with isolated back pain or leg pain, but it is usually both. The sciatica (leg pain) is typically present in one leg only, but occasionally in both. The leg symptoms may manifest as a shooting electricity pain down the buttock, back of the thigh and calf, and into the foot. The sciatica pain may also have a component of numbness, tingling (parasthesia), and/or weakness. Patients may have difficulty sitting or finding a comfortable position because of the pain. In rare instances, a very large herniated disc can cause paraplegia and/or bowel/bladder incontinence. This condition is called cauda equine syndrome when it occurs in the lumbar spine region, and is considered to be a surgical emergency.
Physical Findings
The physical findings for patients with a herniated disc often include lumbar tenderness and spasm, in addition to decreased lumbar range-of motion. Patients are generally in greater pain with sitting and leaning forward. If the spinal nerve compression is severe, it may cause significant numbness (loss of sensation) in the leg or foot and some of the leg muscles to be weak. Deep tendon reflexes may be diminished or absent for the particular spinal nerve that is affected.
Imaging Studies
Plain x-rays of the spine will not show a herniated disc because an x-ray only shows bone structures, not the cartilage disc or spinal nerves. A magnetic resonance imaging test (MRI) is necessary to clearly define the disc injury, and is noninvasive (no needles or dye injection). Before MRI was invented, patients were required to have a CT, myelogram, or CT-myelogram in order to confirm the diagnosis of herniated nucleus pulposus. MRI is now much easier to perform and generally provides better visualization of the disc injury. However, some patients are not able to have an MRI, such as those patients with a cardiac pacemaker, and must have one of the other described imaging tests.
Laboratory Tests
There are no laboratory tests used to diagnose a herniated disc. Occasionally, specific tests are ordered to rule out infection or other causes or back pain and/or sciatica.
Diagnosis
The diagnosis of a herniated nucleus pulposus is fairly straight-forward in most patients. It can be complicated when the symptoms or physical findings are atypical. Some patients will complain of isolated “hip pain” or “knee pain,” and be evaluated and treated for this rather than a back problem. It is important for the clinician to conduct a thorough history and clinical examination prior to formulating a diagnosis so as not to misdiagnosis this condition. Imaging studies (and occasionally laboratory tests) must be used to clarify the diagnosis.
Treatment Options
The treatment for a herniated disc almost always begins with a trial of conservative treatment, which is frequently effective. Deyo and colleagues performed a prospective that showed initial treatment of 2 days bedrest and minimal activity was as effective as 7 days bedrest, and allowed earlier return to work and activity if kept at rest for only 2 days. In addition to rest, other treatments should include oral medications and physical therapy. Anti-inflammatory medications are prescribed most often, and pain medications and muscle relaxant medications should be used for severe pain and muscle spasms. Epidural steroid injections and/nerve root blocks can be performed in patients with severe pain, or if a patient’s recovery has reached a plateau and there is still moderate or severe pain. Greater than 90% of patients with a disc herniation improve with conservative treatment. Studies also show that the size of the disc protrusion generally decreases in size over time. However, patients with severe back and leg (sciatica) pain that fail conservative treatment usually benefit from undergoing surgery and return to normal activities and function. Patients with profound muscle weakness or incapacitating pain may be appropriate candidates for immediate surgery. Ng and colleagues conducted a study that demonstrated improved results if surgery was performed with 12 months from the onset of their symptoms. Microscopic techniques are commonly utilized today, and demonstrate a faster recovery compared with patients treated decades ago.
Selected Bibliography
Deyo RA, Diehl AK, Rosenthal N: How many days of bed rest for acute low back pain? A randomized clinical trial. N Engl J Med 1986;315:1064.
Errico TJ, Lowell TD: The operative treatment of lumbar herniated nucleus pulposus. Curr Opin Orthop 1993;4:115. Frymoyer JW. Back Pain and sciatica. N Engl J Med 1988;318:291.
Garfin SR, Glover M, Booth RE, et al.: Laminectomy: a review of the Pennsylvannia Hospital experience. J Spinal Dis 1988;1:116.
Kelsey JL, White AA III. Epidemiology and impact of low back pain. Spine 1980;5:133.
Kostuik JP, et al.: Cauda equine syndrome and lumbar disc herniation. J Bone Joint Surg Am 1986;68(3):386.
Masui T, Yukawa Y, et al.: Natural history of patients with lumbar disc herniation observed by magnetic resonance imaging for minimum 7 years. J Spinal Disord Tech 2005;18(2):121.
Mixter, WJ, Barr JS: Rupture of the intervertebral disc with involvement of the spinal canal. N Engl J Med 1934;211:210.
Ng LC, Sell P: Predictive value of the duration of sciatica for lumbar discectomy. A prospective cohort study. J Bone Joint Surg Br 2004;86(4):546.
Shapiro S: Cauda equine syndrome secondary to lumbar disc herniation. Neurosurg 1993;32(5):743.
Weber H. Lumbar disc herniation: a controlled prospective study with 10 years of observations. Spine 1983;8:131.