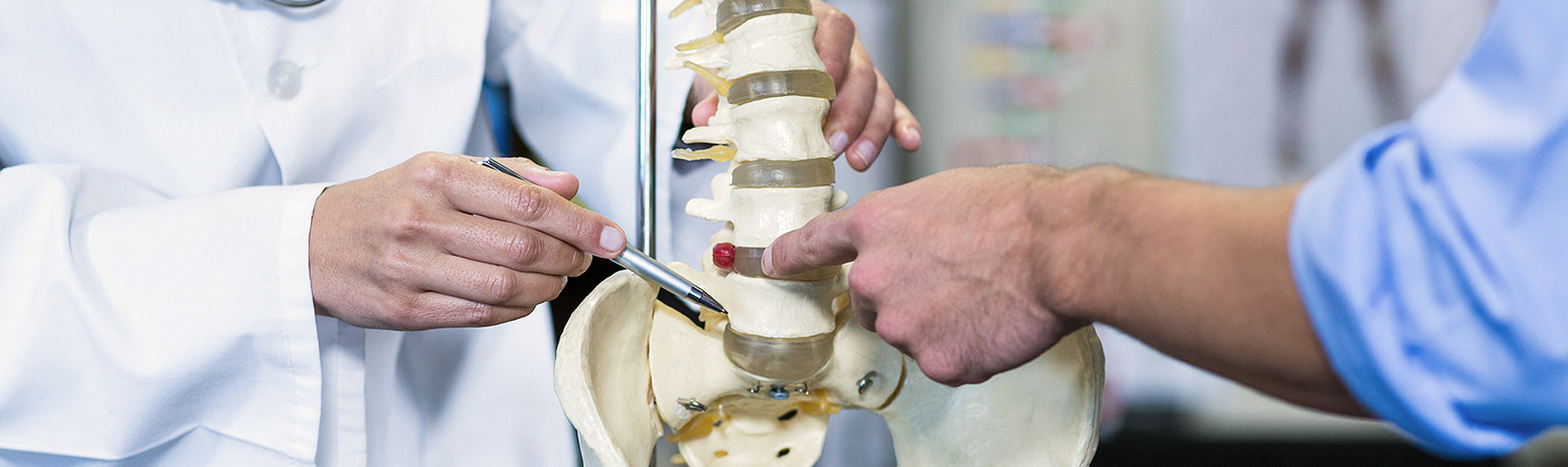
Overview and Indications
Laminaplasty is a unique posterior (back of the neck incision) cervical surgery performed for patients with symptomatic, progressive cervical spinal stenosis and myelopathy. It is performed to open and increase the space for the spinal cord and nerves. It is commonly performed when the majority of spinal compression is in the posterior aspect of the spinal cord. The primary advantage of a laminaplasty is that it does not involve placing a large strut graft and fusing multiple spinal levels together, as compared with an anterior cervical corpectomy and fusion. However, laminaplasty is typically not recommended for patients with cervical disc herniation(s), kyphotic deformity, or instability.
Surgical Technique
The surgery is performed utilizing general anesthesia. A breathing tube (endotracheal tube) is placed and the patient breathes with the assistance of a ventilator during surgery. Preoperative intravenous antibiotics are given. Patients are positioned in the prone (lying on the stomach) position, generally using a special operating table/bed with special padding and supports. The surgical region (neck area) is cleansed with a special cleaning solution. Sterile drapes are placed, and the surgical team wears sterile surgical attire such as gowns and gloves to maintain a bacteria-free environment.
A 4-6 inch (depending on the number of levels) posterior (back of the neck) longitudinal incision is made in the midline, directly over the involved spinal level(s). The fascia and muscle is gently divided, exposing the spinous processes and spine bones. An x-ray is obtained to confirm the appropriate spinal levels. A small cut is made along each side of the posterior (back side) lamina portion of the spine bones. On one side, the cut is complete while on the other side the cut is incomplete and acts like a hinge. This allows the lamina to be opened up like a door, allowing more room for the spinal cord and nerves. A small bone spacer is placed in the opening of the lamina, so that the “door” remains open and heals in this position. A suture or small screw is placed to secure the bone spacer in place.
The wound area is usually washed out with sterile water containing antibiotics. The deep fascial layer and subcutaneous layers are closed with strong sutures. The skin can usually be closed using sutures or staples. A sterile bandage is applied.
The total surgery time is approximately 2-4 hours, depending on the number of spinal levels involved.
Post-Operative Care
Most patients are able to go home 4-5 days after surgery. Before patients go home, physical therapists and occupational therapists work with patients and instruct them on proper techniques of getting in and out of bed and walking independently. Patients are instructed to avoid bending and twisting of the neck in the acute postoperative period (first 4-6 weeks). Patients can gradually begin to bend and twist their neck after 6-8 weeks as the pain subsides and the neck muscles get stronger. Patients are also instructed to avoid heavy lifting in the acute postoperative period (first 4-6 weeks).
Brace
Most patients are placed in a padded, plastic neck brace or cervicothoracic brace (CTO). This reduces the stress on the neck area and helps decrease pain. It can also be used to improve bone healing by maintaining the neck in a rigid position, especially in the first few weeks and months after surgery.
Wound Care
The wound area should remain covered with a gauze bandage secured in place with tape. The area should be kept clean and dry. The bandage should generally be changed every 1-2 days, especially after showering.
Showering/Bathing
Patients can shower immediately after surgery, but should keep the incision area covered with a bandage and tape, and try to avoid the water from water hitting directly over the surgical area. After the shower, patients should change the bandage, and dry off the surgical area. The dressing should otherwise be changed every 2-3 days when at home. Patients should not take a bath until the wound has completely healed, which is usually around 2 weeks after surgery.
Driving
Patients may begin driving when the pain has decreased to a mild level and mobility of the neck has improved, which is usually between 3-8 weeks after surgery. Patients need to be able to turn their neck and body enough to see right and left while driving. Patients should not drive while taking pain medicines (narcotics). When driving for the first time after surgery, patients should make it a short drive only and have someone come with them, in case the pain flares up and they need help driving back home. After patients feel comfortable with a short drive, they can begin driving longer distances alone.
Return to Work and Sports
Patients may return to light work duties as early as 2-4 weeks after surgery, depending on when the surgical pain has subsided. Patients are generally advised to refrain from heavy work and lifting after surgery. Patients may participate in low impact sports and recreational activities after 6-8 months, when the surgical pain has subsided and the neck and back strength has returned appropriately with physical therapy.
Doctor’s Visits and Follow-Up
Patients will return for a follow-up visit to see the doctor approximately 12-14 days after surgery. The incision will be inspected and one suture will be removed. Medications will be refilled if necessary. Patients will usually return to see Dr. Spoonamore every 4-6 weeks thereafter, and an x-ray will be taken to confirm the neck area is stable and healing appropriately. At 8-12 weeks after surgery, patients will be given a prescription to begin physical therapy for gentle neck exercises.
Results and Outcome Studies
The results of laminaplasty surgery in the treatment of symptomatic, progressive, cervical spinal stenosis and myelopathy are generally good. The surgery serves to improve pain and function and prevent further neurologic deterioration and paralysis. Numerous research studies in medical journals demonstrate greater than 83-93% good or excellent results with cervical laminaplsty. Most patients are noted to have gradual improvement of their pain and function following surgery. Although cervical laminaplasty may provide slightly better surgical results with a lower complication rate than anterior cervical corpectomy and fusion, not all patients with cervical spondylotic myelopathy are appropriate candidates for this procedure.
Selected Bibliography
Ebersold MJ, Pare MC, Quast LM. Surgical treatment for cervical spondylitic myelopathy. J Neurosurg 1995;82:745.
Garvey TA, Eismont FJ. Diagnosis and treatment of cervical radiculopathy and myelopathy. Orthop Rev 1991;20:595.
Herkowitz HN. A comparison of anterior cervical fusion, cervical laminectomy and cervical laminoplasty for the surgical management of multiple level spondylotic myelopathy. Spine 1988;13:774.
Herkowitz HN. The surgical management of cervical spondylitic radiculopathy and myelopathy. Clin Orthop Rel Res 1989;239:94.
Hirabyashi K, Bohlman HH. Multilevel cervical spondylosis: laminoplasty versus anterior decompression. Spine 1995;20:1732.
Hukuda S, Mochizuki T, Ogata M, et al. Operations for cervical spondylotic myelopathy: a comparison of the results of anterior and posterior procedures. J Bone Joint Surg Br 1985;67:609.
Kawakami M, Tamaki T, Hiroshi I, et al. A comparative study of surgical approaches for cervical compressive myelopathy. Clin Orthop 2000;381:129.
Kurz LT, Herkowitz HN. Surgical management of myelopathy. Orthop Clin North Am 1992;23:495.
Nurick S. Natural history and results of surgical treatment of the spinal cord associated with cervical spondylosis. Brain 1972;95:101.
Yonenobu K, Fuji T, Ono K, et al. Choice of surgical treatment for multisegmental cervical spondylotic myelopathy. Spine 1985;10:710.
Yonenobu K, Hosono N, Iwasaki M, et al. Laminoplasty versus subtotal corpectomy: a comparative study of results in multisegmental cervical spondylotic myelopathy. Spine 1992;17:1281.