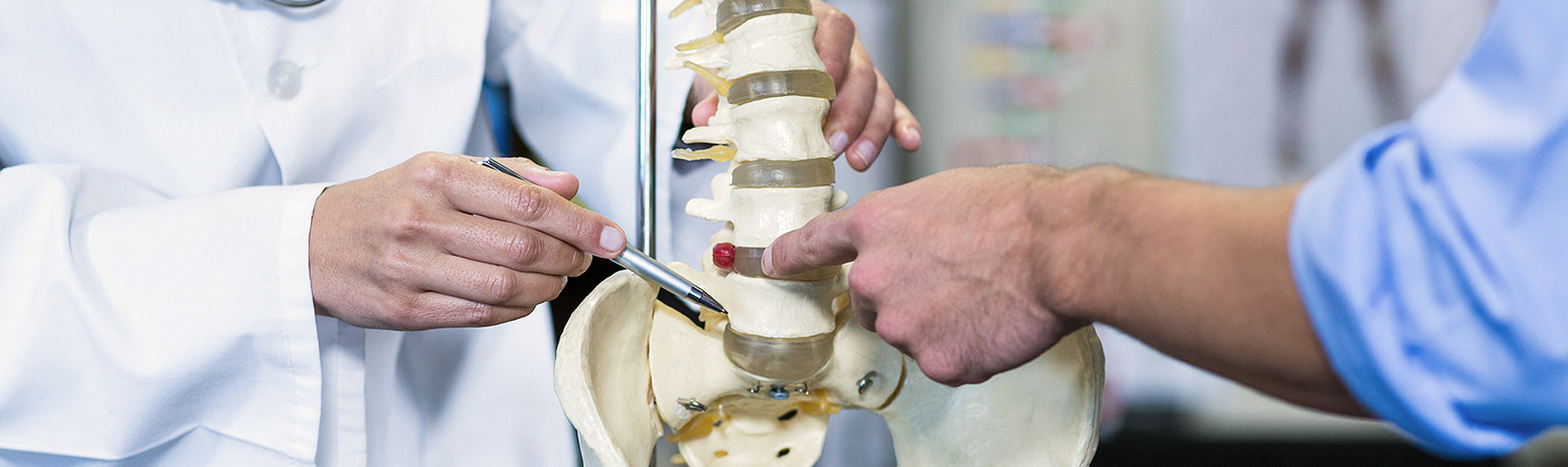
Overview
The term herniated disc describes the condition when the intervertebral disc is injured, and its contents are bulging or protruding into the spinal canal. The terms slipped disc, ruptured disc, bulging disc, disc protrusion, and extruded disc, among others, all mean herniated nucleus pulposus (herniated disc), which is the proper medical term. Although disc injuries and degenerative changes (wear and tear changes as part of the aging process) occur almost equally in both the cervical and lumbar spine, cervical injuries are much less likely to require surgical treatment. However, patients with a severe cervical herniated nucleus pulposus are at risk for injury to the spinal cord, and require careful management.
|
|
Causes
The most common cause of a cervical herniated nucleus pulposus is gradual degeneration of the disc, attenuation (weakening) of the posterior annulus fibrosis, and subsequent protrusion of the nucleus pulposus into the spinal canal causing compression of the nerve root. Sometimes the disc injury occurs suddenly because of an accident or trauma. Most often, however, a cervical disc herniation occurs over time, and patients finally take notice when the neck pain symptoms and/or radiculopathy (radiating arm pain, numbness, and/or weakness) become significant. Although there is an extensive list of risk factors for the development of neck pain (and disc problems), a disc injury can occur in almost any person. A cervical disc injury occurs most frequently in people over the age of 40 years old, and affects men and women equally. The specific cause of a cervical herniated disc injury can often be identified if someone develops severe neck pain and radiculopathy immediately after an accident or injury. However, most people presenting with a disc injury do not recall a specific event that provoked their pain, and the actual cause is indeterminate. People who perform heavy labor (and utilize proper lifting techniques) or participate in sports have nearly the same rate of injury as people who do not.
Symptoms
Patients may present with isolated neck pain or arm pain, but it is usually both when the disc injury is significant. The radiculopathy (arm pain, numbness, and/or weakness) is typically present in one arm only, but occasionally in both. The arm symptoms may manifest as a shooting electricity pain through the shoulder, arm, and into the hand and fingers. The radicular pain may also have a component of numbness, tingling (parasthesia), and/or weakness. Patients may have difficulty turning their head and bending their neck, as it may provoke the radicular pain symptoms. Occasionally, patients will only have significant arm weakness and numbness, but not have any neck or arm pain. In rare instances, a very large herniated disc can cause paraplegia and/or bowel/bladder incontinence, and is considered to be a surgical emergency.
Physical Findings
The physical findings for patients with a cervical herniated disc often include neck tenderness and spasm, in addition to decreased cervical range-of motion. Patients are generally in greater pain if the neck is flexed down and toward the side of the disc herniation. If the spinal nerve compression is severe, it may cause significant numbness (loss of sensation) in the arm and hand and some of the arm and/or hand muscles to be weak. Patients with longstanding nerve compression and muscle weakness may demonstrate atrophy (decreased size) of the affected muscle(s), and this may be quite noticeable when comparing it with the opposite arm. Deep tendon reflexes may be diminished or absent for the particular spinal nerve that is affected.
Imaging Studies
Plain x-rays of the spine will not show a herniated disc because an x-ray only shows bone structures, not the cartilage disc or spinal nerves. A magnetic resonance imaging test (MRI) of the cervical spine is necessary to clearly define the disc injury, and is noninvasive (no needles or dye injection). Before MRI was invented, patients were required to have a CT, myelogram, or CT-myelogram in order to confirm the diagnosis of herniated nucleus pulposus. MRI is now much easier to perform and generally provides better visualization of the disc injury. However, some patients are not able to have an MRI, such as those patients with a cardiac pacemaker, and must have one of the other described imaging tests.
Laboratory Tests
There are no laboratory tests used to diagnose a cervical herniated disc. Occasionally, specific tests are ordered to rule out infection or other causes or neck pain and/or radiculopathy.
Special Tests
Electromyography and nerve conduction velocity (EMG/NCV) tests are useful to determine which nerve is affected, and how severely it is damaged or irritated. The test will often clarify where a nerve is actually being compressed – whether it is in the neck, shoulder, elbow, or wrist. For instance, it can differentiate whether hand and finger numbness is caused by a disc injury in the neck or carpal tunnel syndrome (compression of the median nerve in the wrist).
Diagnosis
The diagnosis of a cervical herniated nucleus pulposus is fairly straight-forward in most patients. It can be complicated when the symptoms or physical findings are atypical. Patients with isolated neck pain may be erroneously diagnosed with a simple neck strain or sprain. Some patients will complain of isolated shoulder pain, arm pain, or hand numbness, and be evaluated and treated for an extremity problem rather than a neck problem. It is important for the clinician to conduct a thorough history and clinical examination prior to formulating a diagnosis so as not to misdiagnosis this condition. Imaging studies (and occasionally laboratory tests) must be used to clarify the diagnosis.
Treatment Options
The treatment for a cervical herniated disc almost always begins with a trial of conservative treatment, which is frequently effective. The primary reason to consider early or immediate operative treatment is when a patient demonstrates profound spinal cord compression from a large herniated disc and has clinical signs of myelopathy and/or spinal cord injury. The natural history of a cervical herniated disc is quite favorable, meaning that the majority of patients improve and do not require surgery. In 1996, Saal published a research study that demonstrated nearly 90% of patients with a cervical disc herniation improved remarkably with nonoperative treatment. Conservative treatments available include rest, ice, heat, chiropractic or physical therapy, medications, neck brace or soft collar, cervical traction, and acupuncture. The most commonly prescribed medications are oral anti-inflammatory medications and pain medications. Muscle relaxant medications should be used for severe pain and muscle spasms, and only for short duration in elderly patients. Complications secondary to medications are more common in the elderly, and all medications should be closely monitored by the prescribing physician. Physical therapy and modalities may also be utilized, primarily to improve a patient’s strength, endurance, and level of function. Manipulation and chiropractic adjustments should be utilized with caution, and may be contraindicated in patients with large disc injuries. Epidural steroid injections and nerve blocks may provide short-term improvement of pain symptoms. Spinal injections are considered immediately for patients with severe, incapacitating pain or patients who have reached a plateau with conservative treatments yet continue to have moderate or severe pain. Surgical intervention is considered when a patient with a cervical herniated nucleus pulposus continues to have pain, weakness, and/or numbness, and has failed conservative modalities. The goal of surgery is to remove the compression from the spinal cord and/or spinal nerves and to improve a patient’s pain and level of function. The preferred surgical treatment is an anterior (front of the neck) cervical discectomy (removal of the disc) and fusion (mending the spine bones together). Generally, a cervical spinal fusion will always be required and recommended in addition to the decompression component, because almost all of the disc will be removed during this procedure. A small bone graft is usually placed between the two spine bones where the disc was removed, so as to restore the normal disc space height and promote fusion. Spinal instrumentation (small metal plate with screws) may also be utilized to impart immediate stability and increase the fusion (bone healing and mending together) rate. In some instances, patients may be candidates for a microscopic posterior (back of the neck) cervical foraminotomy procedure, which can be done using a minimally invasive technique and does not require the spine bones to be fused. This is typically done if the disc injury is small and the nerve compression is primarily due to foraminal stenosis. Regardless of the surgical technique, the outcome is generally excellent with a short recovery period. Patients often have rapid relief of symptoms following surgery and return to work and normal activities within one to three weeks.
Selected Bibliography
Aldrich F. Posterolateral microdiscectomy for cervical monoradiculopathy caused by posterolateral soft cervical disc sequestration. J Neurosurg 1990;72:370.
DePalma AF, Rothman RH, Levitt RL, Hammond NL III. The natural history of severe cervical disc degeneration. Acta Orthop Scand 1972;43:392.
Gore DR, Sepic SB. Anterior cervical fusion for degenerated or protruded discs. a review of one hundred forty-six patients. Spine 1984;9:667.
Grisoli F, Graziani N, Fabrizi AP, et al. Anterior discectomy without fusion for treatment of cervical lateral soft disc extrusion: a follow-up of 120 cases. Neurosurgery 1989;24:853.
Herkowitz H, Kurz LT, Overholt DP. Surgical management of cervical soft disc herniation: a comparison between the anterior and posterior approach. Spine 1990;15:1026.
Krieger AJ, Maniker AH. MRI-documented regression of a herniated cervical nucleus pulposus: a case report. Surg Neurol 1992;37:457.
Kumano K, Umeyama T. Cervical disc injuries in athletes. Arch Orthop Trauma Surg 1986;105:223.
Lees F, Turner J. Natural history and prognosis of cervical spondylosis. BMJ 1963;2:2607.
Lunsford LD, Bissonette DB, Jannetta PJ, et al. Anterior surgery for cervical disc disease. Part I: Treatment of lateral cervical disc herniation. J Neurosurg 1980;53:1.
Maigne JY, Deligne L. Computed tomographic follow-up study of 21 cases of nonoperatively treated cervical intervertebral soft disc herniation. Spine 1994;19:189.
Manabe S, Tateishi A. Epidural migration of extruded cervical disc and its surgical treatment. Spine 1986;11:873.
Murphy MG, Gado M. Anterior cervical discectomy without interbody bone graft. J Neurosurg 1972;37:71.
Palit M, Schofferman J, Goldthwaite N, et al.: Anterior discectomy and fusion for the management of neck pain. Spine 1999;24:2224.
Robertson JT, Johnson SD. Anterior cervical discectomy without fusion: Long-term results. Clin Neurosurg 1980;27:440.
White AA, III, Southwick WO, Deponte RJ, et al. Relief of pain by anterior cervical-spine fusion for spondylosis. A report of sixty-five patients. J Bone Joint Surg [Am] 1973;55:525.