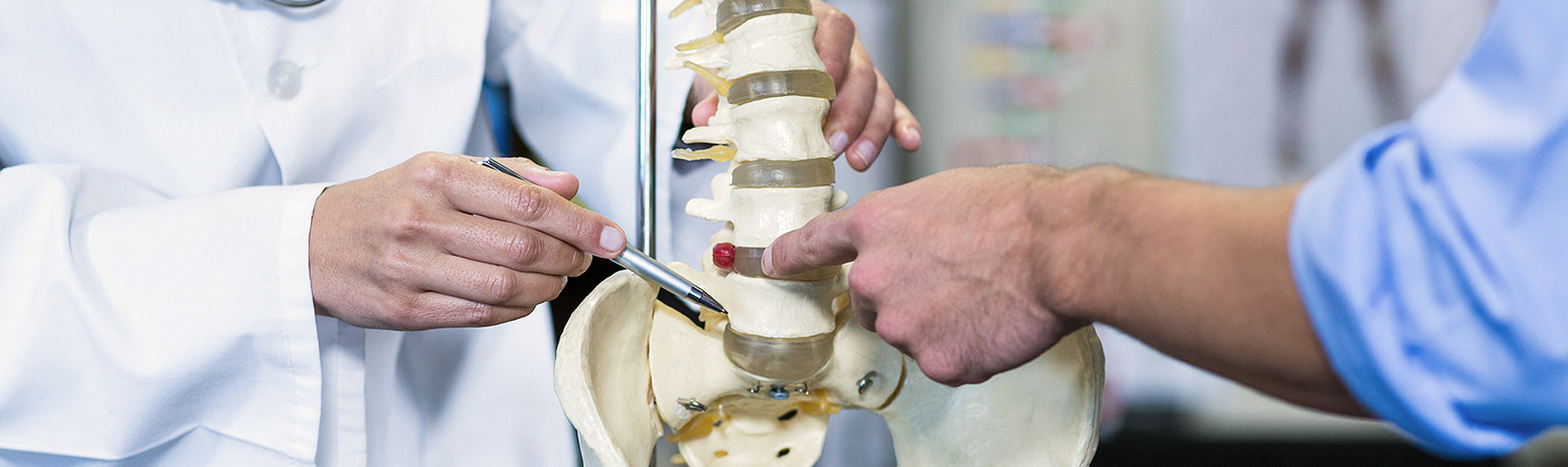
Overview and Indications
Microlaminectomy is performed for patients with symptomatic, painful lumbar spinal stenosis. It is performed to remove the large, arthritic osteophytes (bone spurs) that are compressing the spinal nerves. Most spine surgeons continue to use a rather large surgical incision and exposure without the use a microscope when performing a lumbar laminectomy, which involves a long hospital stay and prolonged recovery period. However, Dr. Spoonamore prefers to perform a microscopic surgical approach using a small, poke-hole incision, with minimal dissection, to accomplish a lumbar decompression of three spinal levels or less. This minimally invasive approach allows for a more rapid recovery, and may provide an improved long-term outcome because there is less muscle and tissue damage.
Surgical Technique
The surgery is performed utilizing general anesthesia. A breathing tube (endotracheal tube) is placed and the patient breathes with the assistance of a ventilator during the surgery. Preoperative intravenous antibiotics are given. Patients are positioned in the prone (lying on the stomach) position, generally using a special operating table/bed with special padding and supports. The surgical region (low back area) is cleansed with a special cleaning solution. Sterile drapes are placed, and the surgical team wears sterile surgical attire such as gowns and gloves to maintain a bacteria-free environment.
A 2-3 centimeter longitudinal incision is made in the midline of the low back, directly over the area of the spinal stenosis. Special retractors and an operating microscope are used to allow the surgeon to visualize the region of the spine, with minimal or no cutting of the adjacent muscles and soft-tissues. After the retractor is in place, an x-ray is used to confirm that the appropriate spinal level is identified.
A complete laminectomy or partial laminectomy/laminotomy (removal of lamina portion of bone) and foramintomy (removal of bone spurs near where the nerve comes through the hole of the spine bone) can be performed, allowing the nerves to return to their normal size and shape when the compressive lesions are removed. The nerve root and neurologic structures are protected and carefully retracted, so that the bone spurs can be visualized and removed. Small dental-type instruments and biting/grasping instruments (such as a pituitary rongeur and kerrison rongeur) are used to remove the arthritic, hypertrophic (overgrown) bone spurs and ligamentum flavum. All surrounding areas are also checked to ensure no compressive spurs or disc fragments are remaining.
The wound area is usually washed out with sterile water containing antibiotics. The deep fascial layer and subcutaneous layer is closed with a few strong sutures. The skin can usually be closed using special surgical glue, leaving a minimal scar and requiring no bandage.
The total surgery time is approximately 1 to 1 ½ hours.
Post-Operative Care
Most patients are usually able to go home 1-2 days after surgery. Before patients go home, physical therapists and occupational therapists work with patients and instruct them on proper techniques of getting in and out of bed and walking independently. Patients are instructed to avoid bending at the waist, lifting (more than five pounds), and twisting in the early postoperative period (first 2-4 weeks) to avoid a strain injury. Patients can gradually begin to bend, twist, and lift after 1-2 weeks as the pain subsides and the back muscles get stronger.
Brace
Patients are generally not required or recommended to wear a back brace after surgery. Occasionally, patients may be issued a small, soft lumbar corset that can provide additional lumbar support in the early postoperative period, if necessary.
Wound Care
The wound area can be left open to air. No bandages are required. Small surgical tapes affixing the suture should be left in place. The area should be kept clean and dry.
Shower/bath
Patients can shower immediately after surgery, but should cover the incision area with a small bandage and tape temporarily, and try to avoid the water from water hitting directly over the surgical area. After the shower, patients should remove the bandage, and dry off the surgical area. Small surgical tapes affixing the suture should be left in place. Patients should not take a bath until the wound has completely healed, which is usually around 2 weeks after surgery.
Driving
Patients may begin driving when the pain has decreased to a mild level, which usually is between 2-10 days after surgery. Patients should not drive while taking pain medicines (narcotics). When driving for the first time after surgery, patients should make it a short drive only and have someone come with them, in case the pain flares up and they need help driving back home. After patients feel comfortable with a short drive, they can begin driving longer distances alone.
Return to Work and Sports
Patients may return to light work duties as early as 1-2 weeks after surgery, depending on when the surgical pain has subsided. Patients may return to heavy work and sports as early as 4-6 weeks after surgery, if the surgical pain has subsided and the back strength has returned appropriately with physical therapy.
Doctor’s Visits and Follow-Up
Patients will return for a follow-up visit to see the doctor approximately 8-10 days after surgery. The incision will be inspected and one stitch will be removed. Patients will be given a prescription to begin physical therapy for back exercises, to start 3-4 weeks after the surgery. Medications will be refilled if necessary.
Outcome Studies
The results of micolaminectomy surgery in the treatment of symptomatic spinal stenosis are generally excellent. Numerous research studies in medical journals demonstrate greater than 86-95% good or excellent results from microlaminectomy surgery, and often show an improved recovery time compared with patients undergoing conventional, open laminectomy surgery. Most patients are noted to have a rapid improvement of their pain and return to normal function.
Selected Bibliography
Albert TJ, Mesa JJ, Eng K, McIntosh TC, Balderston RA. Health outcome assessment before and after lumbar laminectomy for radiculopathy. Spine. 1996;21:960-62.
Kambin P, Casey K, O’Brien E, Zhou L. Transforaminal arthroscopic decompression of lateral recess stenosis. J Neurosurg 1996;84:462-67.
McCulloch JA. Microdiscectomy and microsurgical spinal laminotomies. In: Frymoyer JW, ed. The adult spine: principles and practice. Philadelphia: Lippincott-Raven Publishers 1997:1961-88.
Schaffer JL, Kambin P. Percutaneous posterlateral lumbar discectomy and decompression with a 6.9-millimeter cannula. analysis of operative failures’ and complications. J Bone Joint Surg 1991;73-A:822-31.
Tsou PM, Yeung AT. Transforaminal endoscopic decompression for radiculopathy secondary to intracanal noncontained lumbar disc herniations: outcome and technique. Spine J 2002;2(1):41-8.